Chronic pain, a complex and pervasive condition, affects millions worldwide, posing significant challenges to both patients and healthcare providers. Neuropathic conditions, characterized by abnormal nerve function, present a particularly challenging subset of chronic pain. In recent years, Peripheral Nervous System (PNS) interventions have emerged as a promising solution for targeted relief. PNS involves the modulation of nerves outside the central nervous system to disrupt or alleviate chronic pain signals. This blog post aims to explore the nuances of PNS, providing insights into its mechanisms, effectiveness, and potential benefits for individuals grappling with chronic neuropathic pain.
Understanding Neuropathic Pain
Neuropathic pain stems from damage or dysfunction of the nerves, leading to abnormal signaling and chronic pain. This condition often arises from various factors, including diabetes, infections, or traumatic injuries. Unlike nociceptive pain, which results from tissue damage, neuropathic pain is characterized by malfunctioning nerves that send pain signals in the absence of an apparent injury. Understanding the underlying mechanisms of neuropathic pain involves recognizing the complex interplay of neural pathways and neurotransmitters. It lays the foundation for appreciating how PNS interventions can specifically target and mitigate these aberrant pain signals.
Overview of Peripheral Nervous System (PNS)
The Peripheral Nervous System comprises nerves outside the central nervous system, connecting the brain and spinal cord to the rest of the body. It includes sensory nerves responsible for transmitting signals related to touch, temperature, and pain, as well as motor nerves controlling muscle movement. PNS interventions leverage this intricate network to modulate pain signals and provide relief. The use of electrodes, strategically placed near specific nerves, allows for precise neuromodulation. This section provides a detailed overview of the PNS, emphasizing its role in transmitting sensory information and its potential as a therapeutic target for chronic pain relief.
Mechanisms of PNS for Chronic Pain
The mechanisms of PNS involve the application of electrical stimulation to targeted nerves to modulate their activity. This stimulation disrupts or alters the transmission of pain signals, providing relief for individuals suffering from chronic neuropathic pain. High-frequency stimulation patterns can inhibit pain signals, while other modes of stimulation may induce a tingling sensation that overrides the perception of pain. Additionally, PNS may induce the release of endorphins, the body’s natural painkillers. Understanding these mechanisms is crucial for appreciating why PNS holds promise as a targeted solution for chronic pain.
Types of PNS Interventions
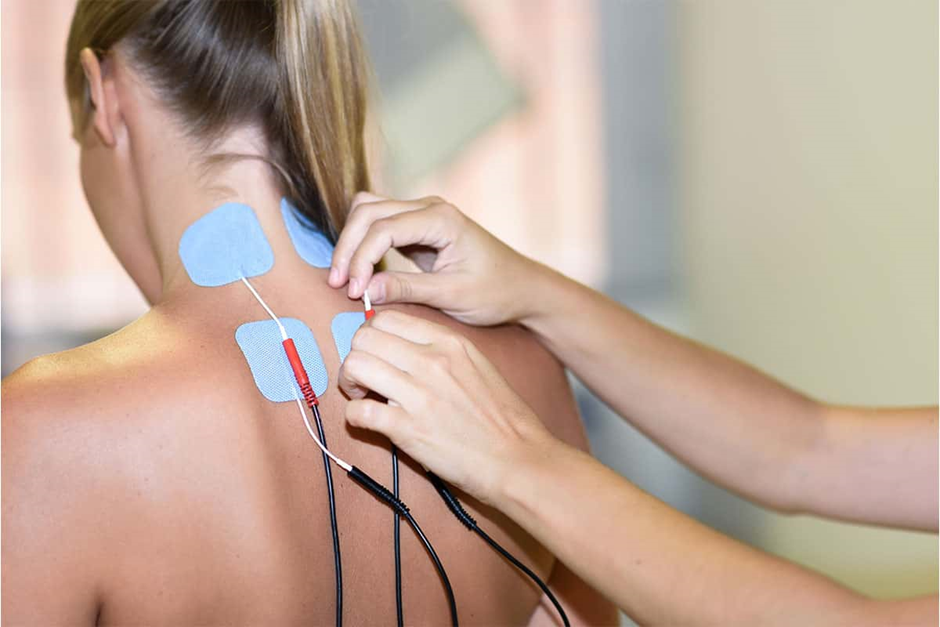
PNS interventions come in various forms, each catering to specific conditions and patient needs. Peripheral Nerve Stimulation (PNS), a traditional approach, involves the placement of electrodes near the affected nerves. High-Frequency Stimulation (HFS) delivers rapid electrical pulses to disrupt pain signals, while Burst Stimulation provides intermittent bursts of stimulation. Sub-perception stimulation is a more recent advancement, delivering stimuli below the threshold of sensation. The choice of intervention depends on factors such as the type of neuropathic pain and individual patient responses. Understanding these distinctions is vital for individuals considering PNS as a potential therapy for their chronic pain.
Effectiveness and Clinical Evidence
The effectiveness of PNS for chronic pain relief is substantiated by a growing body of clinical evidence. Rigorous studies and trials have demonstrated the efficacy of PNS in managing various neuropathic conditions. For instance, research on diabetic neuropathy patients has shown significant reductions in pain scores with PNS interventions. Clinical trials comparing PNS to conventional treatments, such as medication or surgery, underscore the unique benefits of this approach. Real-world examples and patient testimonials further validate the positive impact of PNS on improving the quality of life for those suffering from chronic pain.
Advantages of PNS over Traditional Pain Management
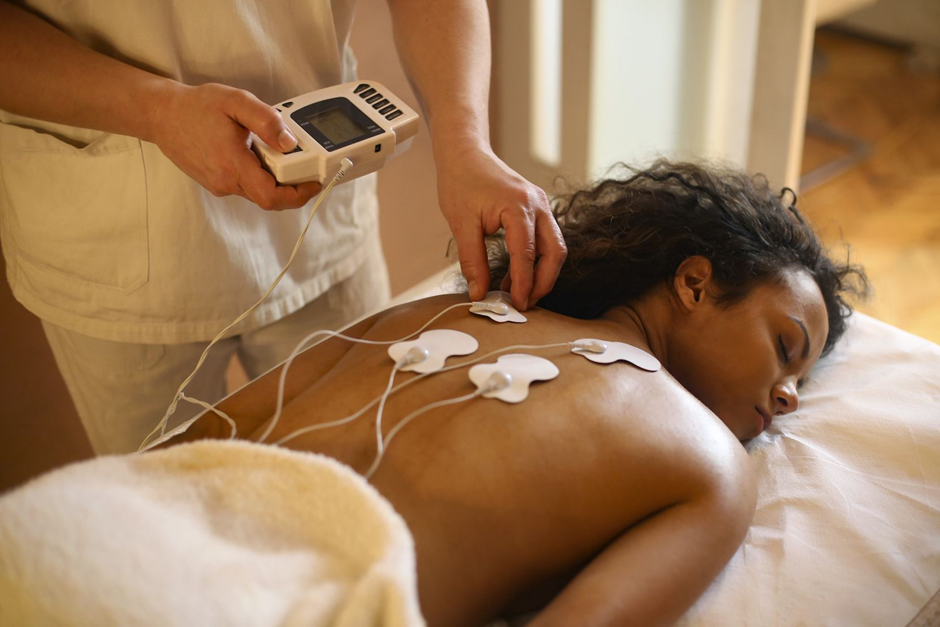
Comparing PNS to traditional pain management approaches reveals several advantages. Unlike medications that may have systemic side effects, PNS offers targeted relief with minimal impact on the rest of the body. Surgical interventions, while effective, often involve greater risks and longer recovery times compared to minimally invasive PNS procedures. Additionally, the ability to adjust stimulation parameters allows for personalized pain management, catering to the unique needs of each patient. Understanding these advantages empowers individuals to make informed decisions when exploring alternatives to conventional treatments.
Potential Risks and Considerations
While PNS presents a promising avenue for chronic pain relief, it’s essential to acknowledge potential risks and considerations. Common side effects may include temporary discomfort at the electrode site or tingling sensations. In rare cases, infection or device-related issues may occur. Candidacy criteria for PNS interventions consider factors such as the type and location of pain, overall health, and patient preferences. A thorough discussion between patients and healthcare providers is crucial to address concerns and set realistic expectations. An informed decision requires a balanced understanding of both the benefits and risks associated with PNS for chronic pain management.
Patient Experiences and Testimonials
The human aspect of chronic pain management comes to the forefront in this section, featuring personal accounts of individuals who have undergone PNS interventions. These stories offer a firsthand perspective on the challenges of living with chronic neuropathic pain and the transformative impact of PNS on their lives. Hearing about the journey from pain and frustration to relief and improved functionality adds a relatable and empathetic dimension to the discussion, emphasizing the potential of PNS to make a meaningful difference in the lives of those grappling with chronic pain.
Future Directions and Research
Concluding the blog post involves looking towards the future of PNS for chronic pain. Ongoing research endeavors focus on refining existing techniques, exploring new stimulation patterns, and developing more advanced devices. The integration of artificial intelligence and machine learning in PNS systems holds the promise of personalized and adaptive pain management. The evolving landscape of PNS encourages readers to stay informed about emerging trends, fostering a sense of optimism for continuous advancements in the field and providing hope for improved solutions for chronic neuropathic pain in the years to come.
Importance
- Targeted Relief: PNS offers targeted relief by directly modulating the activity of nerves involved in transmitting pain signals. This specificity minimizes the impact on surrounding tissues and organs, providing focused relief for neuropathic pain.
- Minimized Side Effects: Compared to systemic medications, PNS interventions often result in fewer systemic side effects. This is crucial in enhancing the quality of life for individuals with chronic pain, reducing the burden of adverse reactions commonly associated with traditional pharmaceutical approaches.
- Reduced Dependency on Medications: The opioid epidemic and concerns about the long-term use of pain medications underscore the importance of alternative interventions. PNS can contribute to reducing dependency on medications, offering a non-pharmacological approach to chronic pain management.
- Improved Functionality: Chronic pain, especially of neuropathic origin, can significantly impair physical and mental functionality. PNS has the potential to enhance overall functionality by alleviating pain, allowing individuals to engage in daily activities and improving their overall well-being.
- Personalized Pain Management: The ability to adjust stimulation parameters in PNS allows for personalized pain management. Tailoring interventions to the specific needs and responses of individual patients enhances the efficacy of treatment, emphasizing the importance of a patient-centered approach.
- Alternative to Surgery: PNS interventions often provide a minimally invasive alternative to surgical procedures. This is particularly relevant for individuals seeking relief from chronic pain without undergoing extensive surgical interventions, reducing associated risks and recovery times.
References:
- https://doi.org/10.1097/j.pain.0000000000000546
- https://doi.org/10.1093/pm/pny071
- https://doi.org/10.1093/pm/pny124
Questions
What is neuropathic pain, and how does it differ from other types of pain?
Neuropathic pain arises from damage or dysfunction of the nerves, leading to abnormal signalling and chronic pain. Unlike nociceptive pain, which results from tissue damage, neuropathic pain is characterized by malfunctioning nerves that send pain signals without an apparent injury.
What is the Peripheral Nervous System (PNS) and how does it relate to chronic pain?
The Peripheral Nervous System comprises nerves outside the central nervous system, responsible for transmitting sensory information. PNS interventions involve modulating these nerves to disrupt or alleviate chronic pain signals, offering targeted relief for neuropathic conditions.
How does PNS work to alleviate chronic pain?
PNS works by applying electrical stimulation to specific nerves to modulate their activity. This stimulation disrupts or alters the transmission of pain signals, providing relief for individuals suffering from chronic neuropathic pain.
What are the different types of PNS interventions?
PNS interventions include traditional Peripheral Nerve Stimulation (PNS), High-Frequency Stimulation (HFS), Burst Stimulation, and Sub-perception Stimulation. Each type has unique applications, catering to different conditions and patient needs.
Conclusion
In conclusion, Peripheral Nerve Stimulation (PNS) presents a promising avenue for treating chronic pain, particularly in neuropathic conditions. Its targeted approach offers a potential for significant relief, improving quality of life for patients who have long struggled with persistent pain, and marks a notable advancement in pain management therapies.
References
- Mayo Clinic – Peripheral Nerve Stimulation (PNS)
- American Chronic Pain Association
- NINDS – Peripheral Neuropathy
- Pain Doctor – Understanding Peripheral Nerve Stimulators
- PubMed – Peripheral Nerve Stimulation Studies
- International Neuromodulation Society
- Spine Universe – Peripheral Nerve Stimulation
- ClinicalTrials.gov – Peripheral Nerve Stimulation Trials
- The Neuropathy Association
- Neurology Advisor – Neuropathic Pain Treatment





